Research project
AMIPS
- Start date: 1st March 2020
- End date: 31st May 2021
- Partners and collaborators: University of Leeds and University of Ghana, Ghana Health Service Funders: NIHR Global Health, Policy and Systems Research Programme
Description
Improving equitable access to essential medicines in Ghana through bridging the gaps in implementing medicines pricing policy
Background
 Ensuring availability and accessibility of medicines and supplies is an important mechanism by which national health systems equitably address the health needs of the population including the poorest and most vulnerable. In Ghana, this is a recognised policy priority. Between 2012 and 2017 the government introduced four policies to improve access to medicines through medicine price regulation, and ultimately health outcomes and quality of life. These policies, currently at different implementation stages, are: (i) supply chain master plan, (ii) framework contracting for high demand medicines, (iii) value added tax (VAT) exemptions for essential medicines and (iv) ring-fencing medicines for local manufacturing. Despite these efforts, medicine prices have remained high and continue to rise. Our core focus is therefore to understand, together with policymakers, why these presumed effective policies are not producing anticipated effects on medicine price reduction.
Ensuring availability and accessibility of medicines and supplies is an important mechanism by which national health systems equitably address the health needs of the population including the poorest and most vulnerable. In Ghana, this is a recognised policy priority. Between 2012 and 2017 the government introduced four policies to improve access to medicines through medicine price regulation, and ultimately health outcomes and quality of life. These policies, currently at different implementation stages, are: (i) supply chain master plan, (ii) framework contracting for high demand medicines, (iii) value added tax (VAT) exemptions for essential medicines and (iv) ring-fencing medicines for local manufacturing. Despite these efforts, medicine prices have remained high and continue to rise. Our core focus is therefore to understand, together with policymakers, why these presumed effective policies are not producing anticipated effects on medicine price reduction.
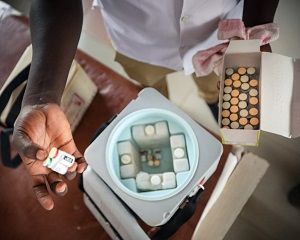
Image above: Malaria pilot vaccine in Ghana © World Health Organization/F.Combrink/2019
Study objectives and questions
Our core question is “Why are these presumed effective medicine price control policies not producing the anticipated effects in implementation in the Ghanaian context?”. More specifically, this project aims to work closely with key policymakers and other stakeholders to:
- Develop an in-depth understanding of major determinants of effectiveness of implementing medicine pricing policies in different contexts
- Develop a shared understanding of main facilitators and barriers to the implementation of medicine pricing policies in the Ghanaian context;
- Drawing on the results of No1 and 2, facilitate: (a) development of a feasible action plan to improve implementation of the four key policies to improve access to essential medicines and (b) co-production of policy-relevant research agenda to address the information needs of key policymakers.
Methods
 The proposed study will comprise two inter-related and overlapping phases. In the first phase, we deepen our understanding of key influences on implementation of medicines pricing policies (a) internationally, through a systematic review of key determinants of effectiveness of implementation of medicines pricing policies and (b) within Ghanaian context, through review of key policy and regulatory documents, prospective participant observations of key policy events and 15-20 in-depth interviews with key stakeholders in a situational analysis of key health systems facilitators and barriers.
The proposed study will comprise two inter-related and overlapping phases. In the first phase, we deepen our understanding of key influences on implementation of medicines pricing policies (a) internationally, through a systematic review of key determinants of effectiveness of implementation of medicines pricing policies and (b) within Ghanaian context, through review of key policy and regulatory documents, prospective participant observations of key policy events and 15-20 in-depth interviews with key stakeholders in a situational analysis of key health systems facilitators and barriers.
Image above: Medicine production in Accra, Ghana (Photo: ILO/Richard Lord/2020 CC License)
The second phase, which will use results from the previous phase, will include series of consultative forums and workshops with key policymakers, managers, practitioners and communities. We envisage organising 5-6 workshops during which we will: (a) share and validate results from the systematic review and the situational analysis and then (b) co-produce, together with key decision-makers, an action plan to operationalise the implementation of the four key policies and an agenda for future research.

Photos from stakeholder workshop in October 2020. © University of Ghana/A.Koduah
Project Impact
 This project is a critical first step in our longer-term plan to improve equitable access to essential medicines in Ghana, through supporting development, implementation, monitoring and evaluation of key policies. The coproduction of research agenda, continuous engagement of key stakeholders are the key to our approach. Through advancing knowledge of implementation barriers and enablers of medicine pricing policies, the study will contribute to improved implementation of medicines pricing policies ultimately to improved equitable access to medicines in Ghana and beyond.
This project is a critical first step in our longer-term plan to improve equitable access to essential medicines in Ghana, through supporting development, implementation, monitoring and evaluation of key policies. The coproduction of research agenda, continuous engagement of key stakeholders are the key to our approach. Through advancing knowledge of implementation barriers and enablers of medicine pricing policies, the study will contribute to improved implementation of medicines pricing policies ultimately to improved equitable access to medicines in Ghana and beyond.
Image above: Accra, Ghana. Photo A. Lew (CC)
Project Team
Nuffield Centre for International Health and Development, Leeds Institute of Health Sciences, University of Leeds:
- Professor Tolib Mirzoev (Joint Principal Investigator)
- Prof Tim Ensor
- Mrs Judy Wright
- Mrs Natalie King
- Dr Anna Cronin de Chavez
- Dr Augustina Koduah (Joint Principal Investigator)
- Dr Irene Kretchy
- Dr Anthony Danso-Appiah
- Dr Leonard Baatiema
Ghana Health Service, Research and Development Division
Project outputs
Articles in peer-reviewed journals
Mirzoev T., Koduah A., Cronin de Chavez A., Baatiema L., Danso-Appiah A., Ensor T., Agyepong I.A., Wright J.M., Kretchy I.A., King N. (2021). Implementation of medicines pricing policies in sub-Saharan Africa: protocol for a systematic review. BMJ Open. 11(2): e044293
Koduah, A., Baatiema, L., de Chavez, A.C. et al. Implementation of medicines pricing policies in sub-Saharan Africa: systematic review. Syst Rev 11, 257 (2022).
Project Briefs
Project information summary: AMIPS - Improving equitable access to essential medicines in Ghana through bridging the gaps in implementing medicines pricing policy
Koduah A, Baatiema L, Agyepong I, Kretchy I, Danso-Appiah A, Cronin de Chavez A, Ensor T, King N, Wright J and Mirzoev T. Implementation of medicines pricing policies to improve equitable access to essential medicines: Insights from four medicine pricing policies in Ghana. Research Brief. 2020 AMIPS Project. Accra, University of Ghana.
Registered Protocol
Mirzoev T, Koduah A, Cronin de Chavez A, Baatiema L, Danso-Appiah A, Ensor T, Agyepong I, Wright J, Kretchy I, King N. The implementation of medicine pricing policies in sub-Saharan Africa: a systematic synthesis of evidence. PROSPERO: International prospective register of systematic reviews. 2020. CRD42020178166
Joint AMIPS/RESPONSE capacity strengthening webinar series on systematic reviews
Materials from further webinars will be available in due course
Further links:
AMIPS website on University of Ghana’s School of Pharmacy
This research was commissioned by the National Institute for Health Research (NIHR) NIHR Global Health Policy and Systems Research Development Award using UK aid from the UK Government (grant number 130219). The views expressed herewith are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.


